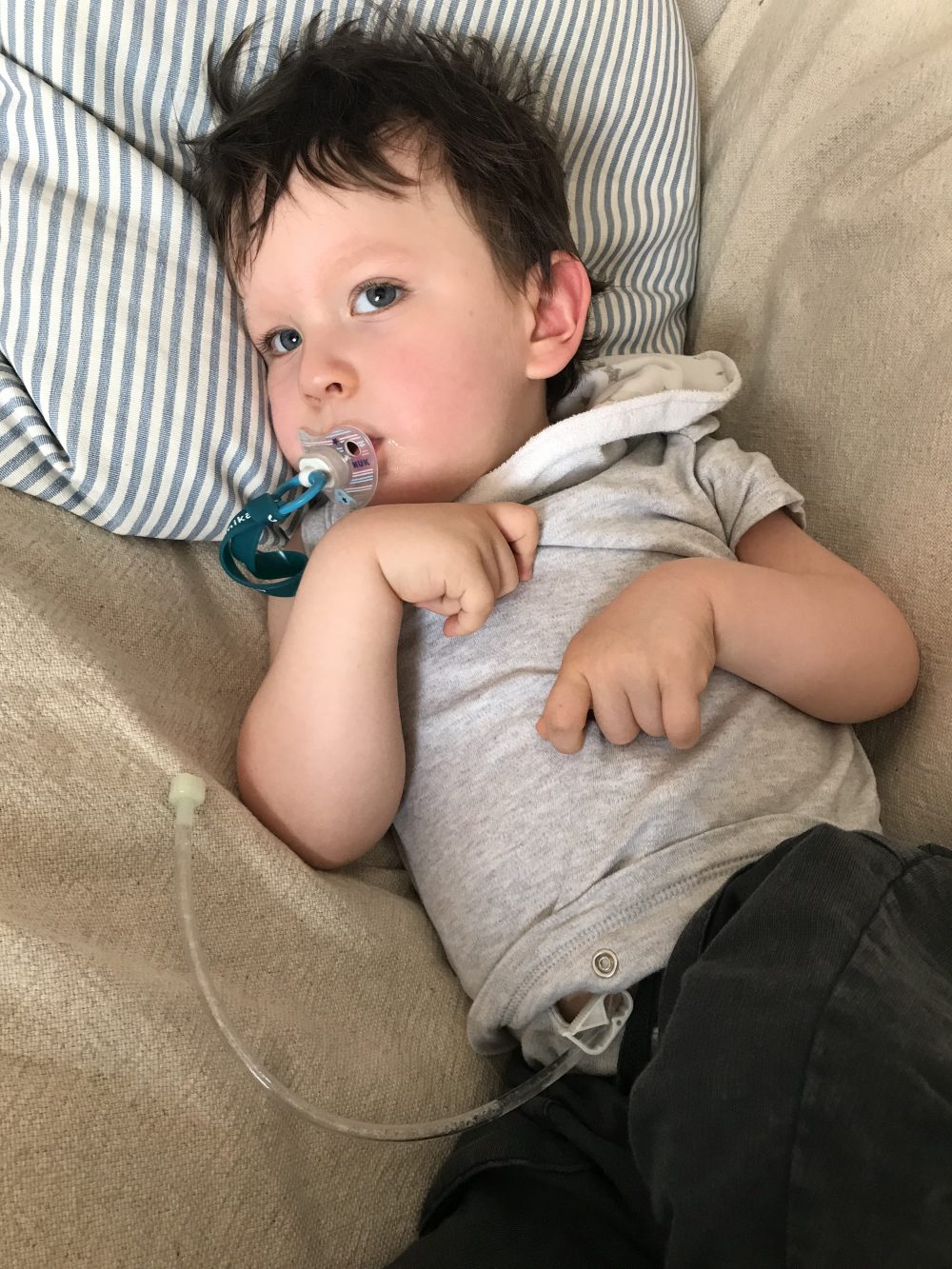
One of the things we fundraised for was for Low Level Laser Therapy (LLLT) When I first heard about QRI from a few NKH Mums – I raised my eyebrows and thought ‘hogwash’. Three months later I was on a train to Birmingham without my guys to learn how to do it. It is a bit… alternative. Very woo-woo. The website is very 90s and the copy on the website is very… holistic and intuitive. For someone who prefers decisive facts and firm science, it was a big leap to get to the point where I was okay to try it on my child.
Now before I get to the point where I’ve joined all the dots – here’s the thing: if there is no harm and there is possible benefits, I’m keen to try it. If it will help Mikaere and it definitely won’t hurt Mikaere, then the risk for trying is low. So we try it. That’s where I started – the possible benefit for Mikaere and his health was 100% greater than the possible risk (because other than time and cost, there is no risk. It’s just light).
So I went on faith. And lots of anecdotal kool aid success stories from other special needs parents.
I got on a train, paid several hundred US dollars and went to learn about a protocol that suggested that with lasers, I might be able to help my son hold up his head.
Here’s how it works. There are a few premises, so let’s start with those.
- The first premise is that cells in our body can take up energy from light. It’s called photobiomodulation. Essentially, there’s a step in the process that makes ATP that has a copper middle. Copper can absorb light in certain wavelengths to give it an ‘energy boost’.The Science, as I understand it: Each cell in our body has a little power factory, called mitochondria. It creates ATP, which is what powers every function in every cell in our body. Cytochrome C Oxidase (CCO) is a step in the mitochondrial electron transport chain – the part that helps make ATP. It transfers one electron (from each of the four cytochrome c molecules), to a single oxygen molecule, producing two molecules of water. At the same time, four protons are moved across the mitochondrial membrane, producing a proton gradient that the ATP synthase enzyme needs to synthesize ATP. CCO has two heme centres and two copper centres. Each of these metal centres can exist in an oxidized or a reduced state, and these have different absorption spectra, meaning CCO can absorb light well into the NIR region (up to 950 nm). Which is to say wavelengths in the red (600–700 nm) and near-infrared (NIR, 770–1200 nm) spectral regions, can be absorbed by the CCO centres, which causes an increase in mitochondrial membrane potential (MMP) above normal baseline levels (increasing the amount of ATP made) and leads to a brief and rather modest increase in generation of reactive oxygen species (ROS) – which is a number of reactive molecules and free radicals derived from molecular oxygen. It’s used in a cell signalling and cell cycling.In a nutshell – given the right wavelengths of light, the mitochondria of a cell can absorb the photons from the laser, which stimulates the cell – increasing the ATP made and improving the signals between cells (amongst other things).
- The second premise is about reflexes. We all have reflexes and they can be retained, preventing development. We all have a number of reflexes designed to help our bodies move through developmental phases. Reflex’s are held in what is called the Reflex Arc – it’s a neural pathway that controls a reflex. Most sensory neurones do not pass directly through the brain, but instead through the spinal cord. This allows for faster reflex actions to occur by activating spinal motor neurones without the delay of routing signals through the brain. When babies grow, the reflex triggers a certain number of movements automatically. These movements pave a set of neural pathways that, eventually, will allow the reflex to be integrated. Once a reflex is integrated, it’s no longer needed and the body will no longer use the reflex.Here’s the important bit: if there is an issue in the brain, or in the central nervous system (like, say because you have Nonketotic Hyperglycinemia) – these reflexes may not be integrated correctly or at all. They might be retained. If a reflex is retained, the child will not easily be able to progress. If they do progress, they’ll need to compensate for the retained reflex.
- The third premise is for reflexes that aren’t integrated can be integrated. Or rather, helped along. If reflexes are typically integrated with repeated movement, repeated, rhythmic movement (or, say, cell stimulation in particular points) may be able to help integrated reflexes by forming neuropathways. Even in brains with neural damage, on the idea that our brains have a certain amount of neuroplasticity, and if possible, they will find a way. This is where things get a bit more… flexible. But, I’m willing to give it a go. Especially because there are so many different success stories from other parents.
And so I went to a workshop held in Birmingham, and I had my first experience of laser therapy.
Woah. Buddy.
I sat through the entire half of the first morning and was so annoyed at myself. I was definitely wasting my time and I’d wasted so much money and I was very very very glad I had not spent thousands of pounds on a laser. The content was way to woo-woo. So far removed from science, and so far removed from what I knew and expected. I half listened, and tried to figure out if I could get a refund on my hotel and a train ticket back to London.
Then the ‘interactive’ part of the session happened. Where you test the reflexes of your partner, do the protocol, and then retest. I was positive I’d feel nothing (it’s just LED lights, I told myself) and that nothing would change.
Here’s the thing. I lay down, and almost instantly the lasers made my body relax even when my brain was still going a million miles an hour. What the heck. I’d never been in a situation where my body was calm and relaxed and my mind was not (it felt very very odd). You could feel your body responding to the lasers, so I kind of relaxed into it. Something was definitely happening, and there must be science behind it. I was sure. I was even more surprised when my reflexes had changed rather dramatically in the test afterwards – profoundly different from the before test.
It’s possible that it was psychoshamtic, but it’s also possible the laser was effective. Hard to know. So I stayed on, and that first night I went on an epic research deep dive. Here’s a small snippet of what I found.
- LED study on that showed significant improvements in executive function and verbal memory of Chronic/Traumatic brain injury patients after LED/near infra-red light therapy. (Source)
- LLLT decreased the muscle spasticity of children with spastic Cerebral Palsy (Source)
- LLLT/photobiomodulation – cells exposed to low-levels of red and near-IR light from lasers or LEDs either stimulate or (less likely) inhibit cellular function, leading to reduction of cell and tissue death, improved wound healing, increasing repair of damage to soft tissue, nerves, bone, and cartilage, and relief for both acute and chronic pain and inflammation. (Source – okay, so not a study, but I got half way through the references before I decided it was probably the most succinct version about LLLT)
- Applying near-infrared light to the head of animals that have suffered traumatic brain injuries produces improvement in neurological functioning, reduces neuroinflammation, and stimulates the formation of new neurones (Source)
- The rats subjected to 500 mW of laser irradiation had a significant decrease in glutamate, aspartate, and taurine in the cortex, and a significant decrease in hippocampal GABA (Source -this one’s helpful, because if there is a decrease in glutamate, the NMDA receptors which glycine binds to are less likely to fire)
They’re mostly the abstracts, because I don’t think I’m allowed to share openly the full studies, but there you go.
We got a laser and we’ve been working it into Mikaere’s routine. Sometimes we manage it, sometimes we don’t. We think we’ve seen some gains, but because we’re doing so much with Mikaere it’s hard to attribute it directly to the laser. We’ll see. I’ll keep you posted.