So. Again yesterday we that quality of life/quality of death conversation. I sat in a room with two Consultants from the PICU and our palliative care nurse from Great Ormond St.
When we had this conversation last time it was in the NiCU at C&W, and our little guy was fine. I couldn’t get into the right headspace because not doing everything we could for our perfect little baby who was awake and beautiful seemed inconceivable.
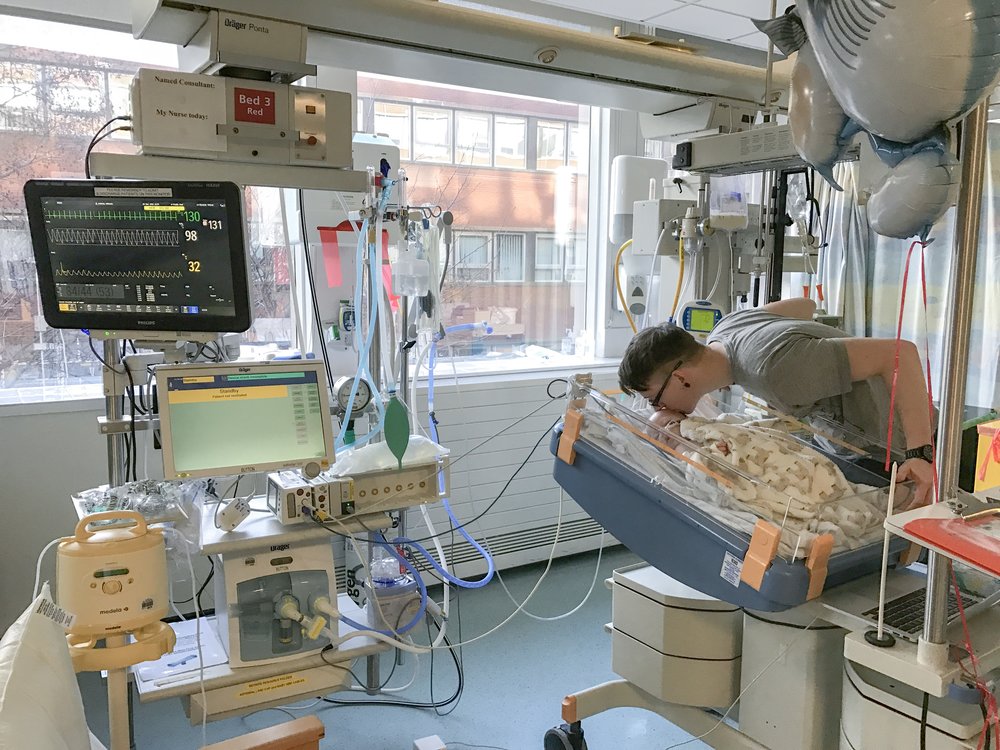
Now my perfect little baby is essentially in a coma, with unknown brain function and one rubbish seizure could rob us of him. What’s more today his seizures are long, 9 minutes, 10minutes, 11 minutes. Long enough that we’re back up on the midazolam we were trying to wean him from.
So, we talk about quality of life, and we talk about his death. I cried. Literally, sobbed. No mother wants to talk about the death of her child, let alone the part where you’re meant to let it happen. Where you do less to prevent it.
Worse, is that Sam wasn’t there, he’s ill today and was on the phone. I sat in a room with three medical professionals and they lead us through a dark, horrid set of questions.
So horrid. Do we ventilate if required? Or do we not? What about CPAP? Having to talk through exactly what level of intervention we would be okay with if things took a turn for the worse is horrid.
After much tears and discussion and internal struggle, we decided that ventilation and CPAP were too much, but oxygen, positioning and suction were okay. The guilt is overwhelming. That we have decided to not do everything possible to prolong his life, and trying to balance that with the sadness that for him, his life may not be pleasant and it would be kinder to not prolong it.
As parents we’re devastated. I hate this. I positively absolutely loathe being in this position. My little baby was fine not even two weeks ago. He was awake, and we were loving on him so so hard. Now he’s in a coma.
Come on babycakes, pull through. We love you so much.
PS I know I keep banging on about it, but we’re still raising funds for NKH research. If our little guy pulls through, any hope of a future is currently at research level. Thank you to everyone, genuinely, who has donated. If you haven’t yet, please consider putting a pound or two in the pot.